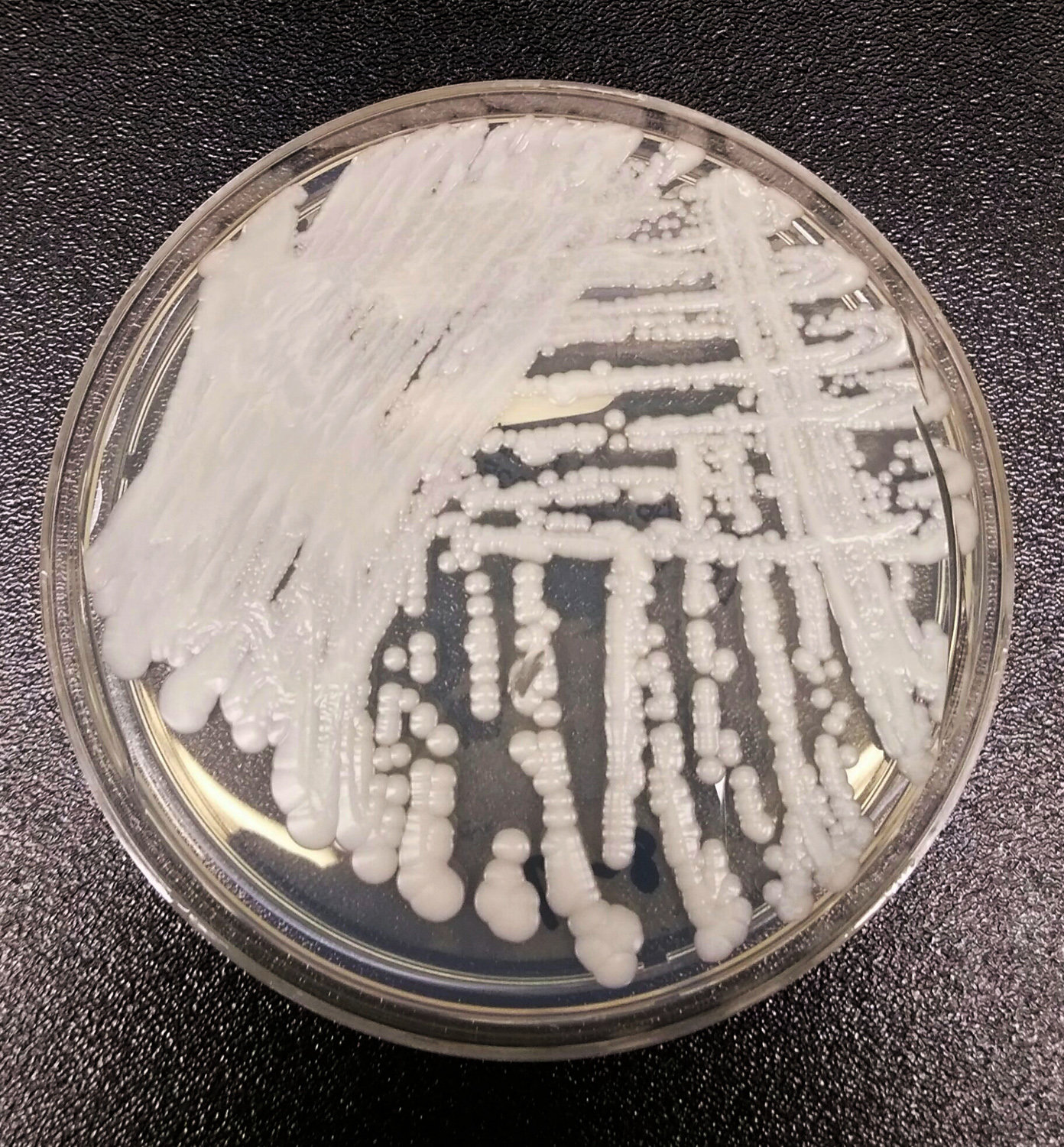
Bronx hospitals battle hard-to-treat bug, C. auris
Nearly a decade ago, a new antibiotic-resistant fungal infection was discovered in Japan. Known as Candida auris, it spread quickly in hospitals and other health care facilities, eventually finding its way across the globe with a stop right here in the Bronx.
That has raised the alarm in New York since C. auris can infect blood streams, the central nervous system, even our internal organs. And yes, it can be fatal.
Last month, the state health department identified 167 hospitals, nursing homes, and long-term care facilities that treated patients either infected with or affected by C. auris.
Seven of those hospitals are in the Bronx, including three under the Montefiore banner in Norwood, Morris Park and Wakefield. Also making the list just across the Broadway Bridge was NewYork-Presbyterian’s Allen Hospital, a popular destination for people living on this side of the borough.
Like many infections, C. auris can live on the skin without infecting the person carrying it. That person would be considered “colonized,” and it is possible for the bacteria to naturally leave the skin without causing an infection, according to Dr. Theresa Madaline, the epidemiologist with Montefiore Health Systems.
C. auris is typically antibiotic-resistant, meaning it doesn’t respond to drugs normally deployed to treat bacterial and fungal infections. When it was first discovered in hospitals in the United States, it was incredibly difficult to remove. The New York Times reported last August that the Brooklyn branch of Mount Sinai Hospital was forced to rip out floor and ceiling tiles to remove traces of the fungus after an infected patient died.
That’s different now, Madaline said.
“The mainstay with Candida and others is bleach,” she said. “That kills organisms very effectively.”
The Centers for Disease Control and Prevention recommends laboratories apply a high-concentration bleach on hard surfaces, allowing it to set before being cleaned off. The ability of C. auris to live on those surfaces without such treatment sets it apart from most other germs, said Nancy Leveille, the executive director at the Foundation for Quality Care, a statewide organization focused on training health care professionals.
“A lot of things don’t live on the surface for very long, like on a tabletop or anything,” Leveille said. C. auris does, however, and because of that, the fungus can easily transfer to someone’s hands when they touch the surface, and then quickly spread to other people who come into contact with that initial person.
While mitigating problem areas could be extensive, tearing up floor tiles was probably more “dramatic” than effective, Leveille said. That likely happened as a result of fear of a new infection soon after C. auris arrived in New York.
“We know how to approach the problem, and we tailor our approach based on the organism itself,” Madaline said. “We’re able to use what we know about resistance from other organisms and apply that to Candida auris.”
Most of the people getting sick from C. auris appear to already be in poor health, according to state health officials, and have been patients in hospitals or long-term care facilities, like nursing homes. Those most at risk have had tracheotomies, are on ventilators, or even receiving some sort of IV-based treatment. Those act similarly to open wounds, allowing the fungus to travel into an already-weakened body.
Symptoms of an infection, according to medical professionals, typically include chills and fever. However, because C. auris has primarily affected people who already are sick, it’s been difficult for doctors to fully isolate the symptoms.
“Normally, your skin is your best defense against fighting infection,” Leveille said. “If it travels in through a port like (a wound), now you’re getting into your internal system. Which, how do you clean that? You clean that with antibiotics.”
Of course, C. auris is antibiotic-resistant, and hard to treat. According to the CDC, more than half the patients who have been infected with C. auris have died. However, Leveille said, it’s hard to say whether most of those people died from C. auris or from other illnesses they already had.
“Having C. auris wasn’t helpful, but wasn’t actually their cause of death,” Leveille said. “And that was hard for them to determine.”
It’s important for public health officials to let the public know that antibiotics are not always needed, Leveille said, and that and over-treating with antibiotics can contribute to more resistance to such treatments — itself a danger.
Pediatricians were some of the first doctors to realize that overprescribing antibiotics could be harmful, she said, as their patients get sick and are prescribed antibiotics more often than adults.
Location-specific antibiotics, like ear drops, can be a better choice than oral antibiotics that spread through the body for certain infections, Madaline said. It’s also important for patients to take antibiotics only as prescribed, and not to share or give antibiotics for friends or family.
While reading about C. auris can be frightening, Madaline says the average person has little to worry about. Hospitals and other medical facilities are safe for them, even if C. auris is present. And they shouldn’t put off any necessary treatment out of fear of being exposed to the fungus.
“I understand why it may feel scary to people when they read about these things,” Madaline said.
“In truth, these resistant organisms, it’s not that they necessarily affect everyone equally. In terms of the average person reading the newspaper who might be at home thinking about this, they’re unlikely to be affected.”